Despite having had a miscarriage between my two children I’ve never questioned my fertility before as I’d innocently taken for granted the ability to have a child if and when I decide to have another. Spending the past six years as a single parent juggling raising my children, working long hours and keeping a home, it’s safe to say that adding to my family wasn’t something that had crossed my mind or taken priority until now. Having met my new partner – who is so adorable with my little ones – we’ve recently had the discussion of moving in together, getting married and having future babies and have established what we both want in life which includes having a child together some day. I’ve always felt that there’s another baby to have, someone we’ve yet to meet, as when my second child was born I didn’t feel the closure that I was expecting and every time I see a baby I feel a great swelling in my heart and longing which has never gone away. But after our close friends personal experiences, my turning thirty and the latest shocking research regarding fertility it seems that it may not be as quick and easy to conceive as we first thought.
Milton Keynes Fertility: Couples Fertility Testing
Oxford and Milton Keynes Fertility in the South East of England is part of the Fertility Partnership which is the largest provider of IVF in the UK and has some of the highest success rates in Europe. Research shows that fertility rates in women noticeably start to decline at the age of 35yrs with only a 5% chance of conception by the age of 40, food for thought as I’m only several months away from my 31st birthday and our cliche 5yr plan of moving in together, getting married and eventually trying for a baby would leave us tight on time to conceive naturally. Sperm count in the West has also more than halved in the past 40yrs and continues to fall at an average of 1.4% each year which can be down to a whole host of factors including lifestyle, diet, stress, sexual health and illnesses in men.
My boyfriend has never fathered a child of his own and as such is unaware of his fertility level, whereas I presumed as I already have children that I could go on having as many as I’d like in life. I had CIN2 precancerous cervical cells removed a few years ago after a routine smear test picked up abnormalities and as such my cervix was cauterised which re-opened a week later causing extensive bleeding and had to be cauterised again. I also have a prolactin hormone imbalance which has led to a lifetime of painful, heavy and irregular periods and a few years ago I bled for two weeks non-stop when my body failed to ovulate so my womb continued to shed its lining until I was medicated. I’ve also had the coil for the past six years since having my second child and went into premature labour multiple times with both of my pregnancies due to a 49 count of Fragile X-Syndrome which is a chromosome disorder, requiring steroid injections whilst also losing blood and an early pregnancy which puts me on the high-risk list for any future pregnancies. In a nutshell, given all of these factors, we wanted to determine if it’s possible to conceive naturally now or in the future, what our options are if conception fails and the benefits and necessity of freezing eggs as a future precaution.

My Boyfriend Provided A Semen Sample For Analysis At Oxford Fertility
So many people wait until they are financially secure, have a new car, big house or have travelled the world and partied away their youth before settling down to start a family; yet when the time comes there is sadly no guarantee that you’ll ever fall pregnant let alone have a healthy happy baby to take home at the end of it. Perhaps knowing the facts sooner precautions could have been taken, tests carried out, eggs frozen or IVF started more effectively at a younger age in order to stand a better chance. Seeing as my children are 10yrs and 6yrs the next few years will involve making a big decision of adding to the family or not. Ideally I would like the children to be close enough in age to grow up together, to have the strength, energy and earning ability to support a growing family and be as medically healthy and safe as possible to sustain a third pregnancy without the mounting risks associated with age. So I’m booked in for a baseline scan and AMH blood test with my partner having a sperm test before we then attend a joint consultation to discover the results of our fertility; peace of mind for our future and the hopes, dreams and plans that we have yet to make.
My boyfriend had an appointment at the Oxford Fertility clinic near Cowley Road in East Oxford to provide a semen sample for analysis and I was able to wait in the waiting room for support. Seeing as the semen sample has to be analysed whilst it is still fresh he attended the Oxford clinic where the lab is whilst our other appointments are based in Milton Keynes. The clinic was very modern, clean and discreet with chilled water and magazines for partners waiting. The waiting room also contains a glass window overlooking the laboratory where staff in white coats operate medical equipment and take notes which was fascinating to watch. Upon arrival my boyfriend was checked in and shown into a private room by a nurse where he provided his semen sample. He explained to me afterwards that the room contained a chair, adult magazines and a compartment where his complete sample pot was to be stowed and a buzzer pressed for the nurse to return to the room in order to bring him back to reception – a very quick and easy appointment before going about the rest of our day.

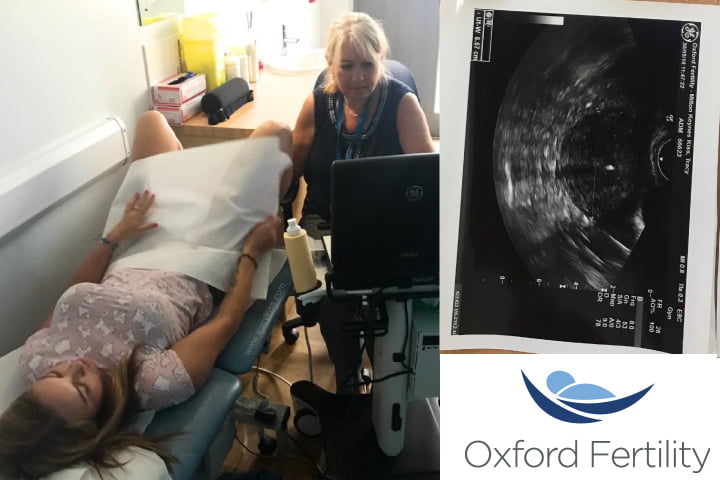
I Attended A Cervical Scan & Blood Test In Milton Keynes
Arriving for my appointment in Milton Keynes I was greeted by a practitioner who showed me into a private room set out as a GP’s office and my boyfriend was present. I took a seat at her desk as we spoke about my previous pregnancies and births, miscarriage and menstrual cycle before she explained what we would be doing. In order to establish my level of fertility I would need to have an AMH blood test to check my hormone levels along with an internal cervical scan. The blood test was just like any other I’ve had, a small scratch on the arm, a single vile of blood taken and then labelled which took all of two minutes. This is the second time that I’ve had a cervical scan as I had irregular bleeding outside of my period several months ago and seeing as my mum had cancer my GP wanted to check me over, however I’ve never had my fertility tested before.
The cervical scan produces images of the uterus and ovaries exactly like an ultrasound during pregnancy but this is an internal scan rather than running a hand piece ontop of the stomach when pregnant. The scan involves using a wand-like device which is wrapped in a condom for hygiene and lubricated for comfort before being inserted into the vagina and manoeuvred into position in order to capture precise images and measurements of the ovaries and womb. Although it may look daunting it isn’t uncomfortable and causes no pain, the wand is slim and long to make it easy to hold and only the tip of it is inserted into the vagina. The scan was performed just like a smear test and I laid on the bed with my legs up and a paper towel across my lap whilst watching the images appearing live on the screen which was fascinating to see. I was told that I have very healthy ovaries with the dark dots of the scan showing 22 receptors on each side as well as the white dot and rod shape confirming my contraceptive coil is still firmly in place and effective. Seeing as I’m not currently looking to conceive I’m happy for my copper coil to remain and this won’t effect my test results as it is non-hormonal.

Oxford Fertility Preservation Prices June 2018
The appointment took around half an hour in total and in a weeks time we’ll return to Milton Keynes to receive our joint test results. Presently we’re both very fit and active individuals, neither of us smoke, we only drink on special occasions and hope to have one or two children together naturally within the next few years. With my irregular periods, previous pregnancy problems and turning thirty I realise my fertility may not be as strong as in my teens and twenties and at the back of my mind I fear having another miscarriage. My boyfriend has concerns from past accidents where he’s been hit in the genitals and occasionally experiences intermittent aching in his testicles along with a very stressful job and struggling to unwind. We recognise the importance of fertility analysis for future family planning and the options available to us both now and in the future and whilst we hope we’ve done everything in our power to lead healthy active lives conducive to extending a family we are emotionally supportive and understanding of one another should we discover otherwise.
UPDATE: Our Fertility Test Results
My mind is frazzled! I never expected to be in this position but we’ve just had the longest discussion in the history of ever whilst driving home from the fertility clinic. Our fertility tests revealed that Freedy has a low sperm count and it’s struck a chord with our plans of having a family together one day as our limits and expectations become all the more prominent now. I’ll try my best to break it down into the contributing factors that we have discussed, the if’s but’s and maybe’s and hypothetical situations and obstacles that we now face. Trying to make sense of this is mind-blowing, yet we’re incredibly relieved to know now rather than later when our chances of conceiving naturally may diminish drastically. If anything I thought I might be the problem, not Freddy.
Given the NHS criteria for being applicable to have free IVF: the female must be below the age of 35yrs, both non-smokers, female BMI must be less than 30, must have been trying to conceive for 2yrs, neither partner must have had children in the past, present or via adoption however if the male has no sperm in their sample they can bypass this criteria. Although we meet the criteria as I have two children already it means that I am not applicable for free IVF on the NHS, instead it would cost us at least £6,000 to attempt to have a child together through private IVF if we fail to do so naturally – funds that not many families may have to hand and aren’t guaranteed to lead to a pregnancy at the end of it.

A Brief Of Our Fertility History
If we wait until I’m 35yrs old to start trying our chances of conceiving naturally become a lot slimmer than they are now. At present the success rate of a fertile young couple (below 35yrs of age) having intercourse 3 times a week in order to conceive across a year is 85%. Due to Freddy’s sperm count of 5.9million per ml (the average fertile range is between 15million-200million per ml) our chances are significantly reduced. Add to the fact that I have irregular periods – meaning less periods per year than the average woman – then we have even less chances to conceive. There is also a 15-20% risk of miscarriage with every pregnancy regardless of conception methods used. Worryingly this figure could be even higher as a lot of early pregnancies go undetected when women fail to realise they are pregnant let alone having a miscarriage; these bi-chemical miscarriages do not show up on a pregnancy scan but instead the HCG hormone in the blood must be monitored to detect them.
We have been together for 7months and without knowing these results would have both wanted to have a child together in the next several years. Now that we have this information which is very much food for thought it has made us consider trying for a baby sooner rather than later into our relationship. If we wait a few years until we’re more financially stable to try to conceive the time may be too late or cost us our life savings and security as a result – something that could have been spent on a wedding, home and future security. Yet if we rush into having a child too soon we sacrifice the earlier care-free days of our relationship and perhaps increase the risk of being single parents to a child with the additional responsibility and strain. As individuals we are certainly heading in the right direction for settling down and starting a family together, yet it feels the start date has been moved far closer than expected, otherwise it may be never at all.

Freddy And I Try To Relax & Unwind Away From Work When Possible
It’s a very individual and difficult decision to make regarding how long you should date or even wait before settling down to begin a family. As I already have two children I know that I’m a capable and independent hard working mother and could easily raise a third child alone if the worst came to the worst, but in a perfect world I wouldn’t want to. I would like a happy marriage, loyal husband and kind father to all of my children. I believe I’ve finally found that, yet it’s still early days for us and anything could happen. A relationship is typically based upon spending several hours or more a week with each other, you could have a year long relationship and only spend weekends together, or a year long relationship and spend everyday together and know one another inside out. The time could be quality or quantity but does it necessarily make a couple more likely to stay together or not when a baby is involved? I think my fear of being a single parent has certainly prevented me from dating for a long time, let alone considering having more children until now. I adore children, love my family and have always felt the desire to have more but are we ready now as a couple or will we ever be as ready, young and capable as we are now? It’s an emotional, mental, physical and financial tug of war for us both and something we thought we’d have years to decide upon. Yet we are both glad that we know the results of our fertility soon enough to make an informed decision about our future without having waited another 5yrs to have found out when our chances of having a child together would be significantly lower, if not naturally impossible.
This information takes time to process and understand the true weight of the consequences and it’s hard to know what to feel right now. Personally this ‘now or never’ scenario is something I never expected to be faced with. Beforehand I had the ignorance of thinking that time would always be in my favour, that I could meet the man of my dreams, fall in love, buy a puppy and live happily ever after with as many children as my heart desired. But the expectations you have of life are never guaranteed and we have to now find acceptance and understanding of our circumstances as a couple and family. Which, had we both been with different partners the results may not be the same as they are for us both today. If Freddy had met somebody younger or without children of their own he may have more time and NHS funding to decide on when is best to become a first time father. Likewise if I were with with a partner with a higher sperm count immediate fertility may not be an issue for me and I could happily wait until I’m 40 or even older to have another child. In this sense every couple is unique, every circumstance individual and every life on this earth a true blessing when you realise what it takes to have a child. It makes me feel incredibly humbled to already have two healthy, wonderful and kind children of my own. As much as we’ve discussed having children together one day we also have to consider the prospect of never being able to have children together, for Freddy never to be a father which makes my heart ache. The best case scenario however is simply a delay in falling pregnant, removing my contraception and spending months if not years attempting to conceive naturally, maybe having just the one child together instead of the two or possibly three we’d have wanted – all things to consider in time as we play devils advocate.

We Like To Keep Fit, Healthy & Active Together
We’ve discussed the strengths and weaknesses of trying for a baby in the near future to assess our situation and have recognised we would both like to have a child of our own, welcome the intimacy of trying to conceive, the children are open to having a new baby brother or sister and seeing as we’re already a family we are equipped and capable of raising another child with little disruption to our everyday lives. As I work from home it wouldn’t effect my ability to support the family, yet the immediate con’s of having a baby now would be the additional financial strain, the emotional risk of not being able to conceive or having another miscarriage and the potential for friends and family not being accepting of our decision as we’ve known each other for less than a year. Having a baby could also lead to a strain on our relationship and heighten the risk of us breaking up as tiredness, hormones and stress can increase, if we fall ill or have complications we may be unable to work and risk losing our home and there is the possibility of having another autistic, mentally or physically disabled child.
Considering all of these factors, if we decide to try for a baby then in order to fall pregnant I would first have to have my copper coil removed which would take place during my next period to ensure that I wasn’t already pregnant, as whilst it’s a very secure form of contraception it is still possible to conceive with the coil in place. Contraceptives such as the coil, the pill and implant are the quickest form for fertility to return once they have been stopped or removed, however the injection can take around 6months. It takes around 12 months for a couple to try to conceive naturally, as cycles and sperm must be alive and present at the right time, and after 2yrs of trying to conceive without falling pregnant the ovaries and tubes are usually checked for blockages as a possible cause. Our heart-to-heart has revealed that Freddy would like to become a father by the age of 31, at which time I would be 34 and this keeps us just within the 35yr fertility drop for women which gives us our best chance of conceiving naturally and means for our relationship that we would have been together for just over four years. My youngest child would be 9yrs and my eldest 14yrs which is quite an age difference but equally ideal for independence and childcare. It’s something that we don’t want to stress about right now but instead let nature take it’s course as and when the time comes. I would therefore look to have my coil removed in two years time when I turn 33 which we both feel is a reasonable amount of time.

My Daughter Is An Articulate, Creative And Considerate Young Lady
To improve Freddy’s sperm count he can begin taking WellMan supplements before trying to conceive which include zinc, selenium and antioxidants. He should avoid having hot laptops on his lap or sitting in hot cars as this will raise the temperature of the testicles and effect the sperm. As he’s a non-smoker he’s already in good health and cutting down on alcohol is also recommended. The frequency of ejaculation doesn’t reduce the quality of sperm, just the volume and it’s the quality that is key; therefore withstanding from intercourse prior to my period won’t improve our chances of conceiving. It’s suggested couples have intercourse three times a week when trying to conceive as sperm can survive for a few days at a time and this maximises the chances of fertilisation. Contrary to popular belief, a low sperm count doesn’t effect testosterone levels. Men can be born with a low sperm count genetically, lower their count because of lifestyle choices, infections, injuries and STI’s which can cause testicular inflammation but have no long term effects on fertility once treated. When we decide to begin trying for a baby it’s recommended that Freddy returns for another sperm test to check the count as sperm takes 80days to produce, so how he lives today will effect the sperm he ejaculates in a few months time and his count may well be higher for the next test. For this reason lifestyle changes and healthier living take time to take effect. Funding for IVF on the NHS (which we are not applicable for) takes time and varies from area to area. Groups of local GP’s are given a pot of money each year and have to decide on how best to spend it and which areas to fund. IVF is decided locally for funding and changes year to year; in Oxford where we had our testing, funding for IVF is limited to one NHS cycle if all of the criteria is met, however Scotland provide three NHS cycles but the waiting list is much longer.
A ballpark figure for the cost of one IVF cycle is around £6,000.00 and can be dramatically higher depending on the quantity of expensive drugs involved which will vary depending on the condition of the ovaries and the treatment necessary which takes place in a laboratory. 50,000 sperm must be mixed with each individual egg it in order to have to best chance of fertilisation. Ten eggs are typically used at a time per IVF cycle which may be out of immediate reach for men with low sperm counts. In this case multiple visits can be made in order to collect and freeze sperm until these figures have been met. The average sperm count of a fertile man is 15million-200million per millilitre, with a single ejaculation measuring between 2-6ml. However 32% of this amount is lost to mortality rate as not all swimmers move forwards, a further 4% suffer from morphology where the shape is unbalanced and may have multiple heads and tails, therefore many sperm are lost, wasted or unsuitable for the egg. For Freddy his 5million count is below average but the quality of his sperm is very healthy and capable of fertilisation. ICSI or Intracytoplasmic Sperm Injection is a technique invented in the late 1970’s that allows for a single sperm to be injected into a mature egg. In severe cases where 5 out of 15million sperm are useable those with two heads or an inability to swim are rejected and a healthy, strong sperm individually selected in a laboratory. The tail is removed to prevent it from swimming away and it is injected directly into the egg which costs between £1,000-£1,500 at a time. There is the argument that this prevents natural selection from happening however the strongest fastest swimmer is the most likely to reach fertilisation and this speeds up the process. The NHS cover both sperm freezing and ICSI methods for qualifying couples dependant on their needs. If a baby is conceived through IVF during a cycle then the additional eggs and sperm already collected can be kept in storage should future children be desired. Frozen embryos are easier and more cost effective to come back to rather than beginning the collection process again and with advanced technology the survival rates are just the same at 95%.

My Son Fills Our Days With Sunshine & Surprises
Women should ovulate naturally every 3-5wks, however the ovaries can be stimulated with medication to increase regulatory. As well as a blood test, the ovaries are scanned for the number of follicles as well as checking the womb for polyps and fibroids which can prevent the embryo from implanting. Polycystic Ovaries Syndrome or PCOS refers to irregular or no menstrual periods, heavy periods, excess body and facial hair, acne, pelvic pain, difficulty getting pregnant, and patches of thick, darker, velvety skin and may also cause a problem. I have been checked against all of these and thankfully my ovaries are clear and healthy which means my fertility falls within the female average. The goal of IVF is to take a single pregnancy to full term, however twins can be requested if acceptable. The risk of a multiple pregnancy must be fully understood as mortality rates are higher as well as complications. Where multiple eggs are used to create embryos for pregnancy, not all eggs and sperm will continue to develop and survive, so on average just one embryo is put into the womb but 1-2 may be selected in the UK with exceptional circumstances allowing for 3. In America multiple pregnancies are less regulated and therefore multiple embryos are implanted into the womb at the same time in order to increase chances yet pregnancy complications and risks dramatically increase and many babies are born at 20wks because of this, often passing away shortly after.
The advice we have been given as a couple is that my ovaries are in a healthy condition and I have a good reserve of eggs so time is not of the essence for me until I reach 35yrs and my fertility rate begins to drop, which is followed again at 37 and 40 and would then put me outside of the parameter for IVF. Stress can have an impact on sperm count, however the extent of it is yet to be measured. The average couple looking to conceive with a normal sperm count and healthy ovaries has an 85% chance of falling pregnant within 12 months of trying. Of the remaining 15% of couples, 50% of these will conceive within 2yrs and the other 50% will be unable to conceive naturally. Therefore with Freddy’s low sperm count our chances are below average, even more so with my irregular periods and the time limit on my fertility with age. With Freddy’s age sperm quality will also decrease as the risk of having a child with ADHD and ASD increases. The main factor in the success rate of IVF is the females age – below the age of 37yrs the success rate of IVF is 35%. Overall we fall into the minority of couples trying for a child which may increase the time that it takes for us to conceive or prevent us from ever conceiving naturally, it’s impossible to tell which it will be. However by the age of 32yrs, if we allow 2yrs of trying for a baby and haven’t fallen pregnant then we would consider starting IVF. As each IVF cycle takes 6-7wks this would give us one year to have multiple cycles before I reach the age of 35 and my fertility drops. Until that time we’ll continue living, loving and raising our beautiful family whilst being grateful for the time and memories that we make and share together; a reminder to never take life for granted.
UPDATE: Sperm Retest Results November 2018
Seeing as six months had passed since finding out about Freddy’s low sperm count we felt that his change in lifestyle choices had been long enough to warrant a retest in his sperm count. It was important to us to have a final answer on the state of his fertility in order for us to think about having a future family or accepting our present circumstances and remaining as we are.
In our heart of hearts we were hoping that cutting back on drinking, quitting occasional smoking, taking a daily multivitamin for men, reducing processed foods and eating more fruit and vegetables would make a difference to Freddy’s sperm count. He’d also been conscious not to sit down as much and to keep more active, as well as removing his laptop from his groin and placing it on the table as heating up the testicles isn’t recommended – he also limits the use of his heated seat whilst driving. Our aim was to reach the minimum of 15million sperms per ml, but the results were beyond shocking!

Upon Making Lifestyle Changes Freddy Improved His Spermcount Tenfold
As you can see from this letter we received from Dr Tim Child, at our results consultation we were given the news that Freddy’s sperm count has increased wonderfully:
-Freddy’s sperm volume has increased from 2.5ml to 5ml per ejaculation
-Freddy’s sperm count has increased from 5.9million per ml to 51million per ml
-Freddy’s motility (ability to swim towards the egg) has increased from 45% to 71%

Tim Childs, Kay Burley, Tracy Kiss & Freddy Shaw For Sky News
Because of this Freddy was asked to speak on Sky News with presenter Kay Burley and Dr Tim Child during fertility week to encourage men to make healthier lifestyle choices to naturally increase their fertility where possible.
We are absolutely over the moon with the outcome as it means we now stand a far higher chance of conceiving naturally as and when we choose to and no longer have an impending time limit or additional stress to have a baby before it’s too late. It means that we can spend more time planning, preparing and waiting until the time is right for us both rather than making hurried decisions. It’s given us the freedom to let nature take its course – something we wish for all couples and hope that speaking out about this will help others to live healthier, happier lifestyles that makes them feel good, boosting their fertility as a bonus.
www.oxfordfertility.co.uk
Facebook: /OxfordFertility
Twitter: @OxfordFertility
Instagram: @OxfordFertility

